Is Your Headache Actually a Neck Problem? Understanding and Relieving ‘Tech Neck’ in Sungai Buloh
If paracetamol cannot fully resolve your persistent headaches, your skull is likely not the origin. For corporate employees in Sungai Buloh and the Klang Valley, cervicogenic headache from Tech Neck is rapidly becoming the defining occupational health complaint of the decade.
Consult a Verified Sungai Buloh Physiotherapist
If you suffer from persistent headaches that paracetamol cannot fully resolve, your skull is not the origin of your pain. In the majority of cases, the true source is cervicogenic headache — a headache originating from the muscles, joints, and trigger points of the cervical spine (your neck). For corporate employees and home-office workers in Sungai Buloh and the greater Klang Valley, this is rapidly becoming the defining occupational health complaint of the decade.
What Exactly Is “Tech Neck” and Why Is It an Epidemic in Malaysian Offices?
Tech Neck is a repetitive strain injury caused by sustained forward-head posture during prolonged use of screens, smartphones, and laptops. For every 2.5 centimetres your head shifts forward from its neutral position above your spine, the effective load on your cervical vertebrae increases by approximately 4–5 kg. At a typical working posture, your neck muscles are managing the equivalent of a 20–27 kg load — all day, every day.
In Malaysia, several compounding factors make this condition particularly aggressive (and frequently overlap with conditions requiring non-surgical carpal tunnel relief in the Klang Valley):
- Work culture: Long office hours in Sungai Buloh’s industrial and commercial zones, combined with the normalization of “WFH setups” on dining tables and sofas, produce chronically poor ergonomics that fail Department of Occupational Safety and Health (DOSH) Malaysia guidelines.
- Dual-screen fatigue: Corporate employees managing multiple monitors often develop asymmetrical muscle tension, triggering unilateral (one-sided) headaches.
- Air-conditioning dependency: Malaysia’s tropical heat means offices and home offices are perpetually air-conditioned. Cold, dry air from prolonged AC exposure causes superficial muscle stiffness in the cervical and upper trapezius region, worsening existing tension.
- High smartphone usage: Malaysia consistently ranks among the highest globally for average daily smartphone screen time, adding hours of downward neck flexion on top of already strained work postures.
The result: A population of workers with chronically overloaded suboccipital muscles, upper trapezius trigger points, and compressed cervical facet joints — all of which directly refer pain into the skull, producing what feels exactly like a conventional headache.
How Do You Know If Your Headache Is Coming From Your Neck?
A cervicogenic headache has specific clinical features that distinguish it from migraines or tension-type headaches of purely vascular or neurological origin. If your headache matches three or more of the following criteria, your neck is almost certainly the primary driver:
Location
Pain typically begins at the base of the skull (occiput) and radiates forward over the top of the head, behind the eyes, or into the temples.
Trigger
The headache reliably worsens or is provoked after prolonged desk work, driving, or looking down at a phone.
Stiffness Accompanies Pain
You notice reduced neck rotation or a feeling of “tightness” before or during the headache episode.
Unilateral Presentation
The headache is predominantly on one side, correlating with which side you hold your phone or which direction your monitor is positioned.
Painkiller Resistance
Paracetamol or ibuprofen provide only partial, temporary relief — the headache returns once medication wears off because the structural cause is untreated.
Point Tenderness
Pressing on specific spots at the top of your neck, the base of your skull, or between your shoulder blades reproduces your familiar headache sensation — the clinical hallmark of myofascial trigger points.
Malaysian clinical note: If your headaches are accompanied by visual disturbances, nausea, or neurological symptoms (numbness, weakness in limbs), consult a registered medical practitioner or neurologist first to rule out primary pathology before pursuing manual therapy.
What Are Trigger Points and Why Do They Cause Headaches?
Trigger points are hyperirritable, contracted nodules within a muscle’s fascia that generate referred pain patterns far from their actual location. Think of them as “electrical fault points” in your muscular system — a tight knot in your upper trapezius does not just hurt locally; it sends a predictable referred pain signal into your temple, jaw, or behind your eye.
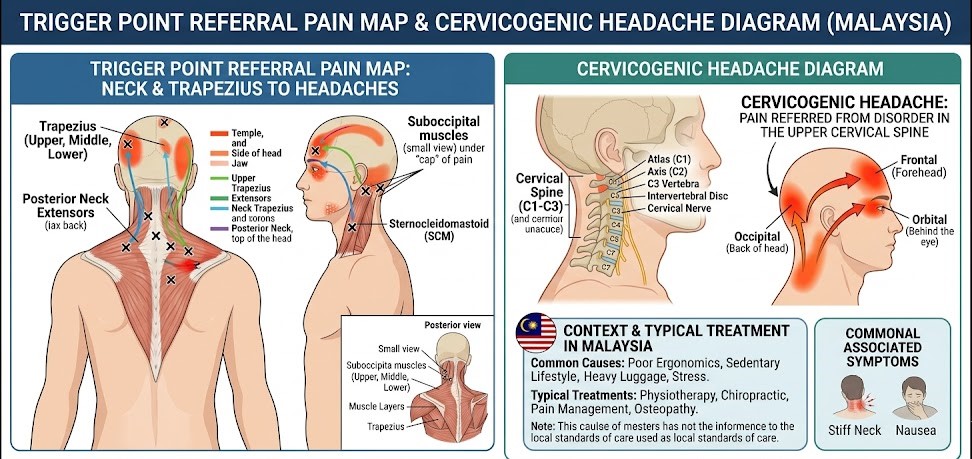 Key trigger point locations in the neck and upper back, and their referred pain patterns into the skull — the anatomical basis of cervicogenic headache.
Key trigger point locations in the neck and upper back, and their referred pain patterns into the skull — the anatomical basis of cervicogenic headache.The key muscles generating headaches in tech neck sufferers are:
| Muscle | Location | Referred Pain Target |
|---|---|---|
| Suboccipitals | Base of skull | Top and front of skull, behind eyes |
| Upper Trapezius | Neck/shoulder junction | Temple, side of head |
| Sternocleidomastoid (SCM) | Side of neck | Forehead, behind ear |
| Levator Scapulae | Neck to shoulder blade | Neck and upper back |
| Splenius Capitis | Back of neck | Top of skull |
These trigger points do not resolve on their own through rest, stretching, or over-the-counter medication. They require direct, targeted mechanical intervention to release the contracted sarcomere clusters and restore normal muscle function.
What Is Trigger Point Release Therapy and How Does It Work?
Trigger Point Release is a manual therapy technique in which a trained therapist applies sustained, calibrated ischemic compression directly to the trigger point nodule to mechanically disrupt the contracted tissue and restore blood flow to the area. The process forces the hypoxic (oxygen-deprived) muscle fibres to release their contraction, immediately reducing referred pain.
For cervicogenic headache, an experienced therapist will systematically address the entire myofascial chain — not just the most painful spot. This typically involves:
- Assessment: Mapping active trigger points by palpating the suboccipital group, upper trapezius, SCM, levator scapulae, and splenius capitis to confirm which muscles are generating the referred headache pattern.
- Ischemic Compression: Applying sustained thumb or elbow pressure directly to the nodule for 30–90 seconds until the referral pattern diminishes and local tissue resistance releases.
- Dry Needling (where indicated): Inserting fine acupuncture-gauge needles directly into the trigger point to elicit a local twitch response — considered the most effective mechanical method for releasing deep suboccipital trigger points that are inaccessible to manual pressure.
- Post-Release Stretching: Gentle cervical flexion, rotation, and lateral flexion stretches performed immediately after trigger point release to restore resting length and prevent rapid re-activation.
- Cervical Joint Mobilisation: Graded manual mobilisation of the C1–C3 facet joints to restore articular mobility and reduce the proprioceptive irritation that sustains the trigger point cycle.
- Home Programme: A structured self-care protocol including suboccipital release with a therapy ball, chin-tuck posture correction, and ergonomic workspace modifications tailored to the patient’s Sungai Buloh office or WFH setup.
Suffering from Headaches That Won’t Respond to Painkillers?
Our vetted physiotherapy partners in Sungai Buloh and the Klang Valley specialise in cervicogenic headache and Tech Neck rehabilitation — accurate diagnosis and hands-on treatment from your very first session.
Book Tech Neck Rehab in Sungai BulohPhysiotherapy Treatment Protocol for Tech Neck & Cervicogenic Headache
A comprehensive Tech Neck rehabilitation programme combines manual therapy for immediate symptom relief with corrective exercise and ergonomic retraining to prevent recurrence — the two goals must be addressed in parallel for lasting results.
Hands-On Clinical Treatment
- Trigger point release — ischemic compression of suboccipital, upper trapezius, and SCM trigger points to immediately reduce referred headache
- Dry needling — highly effective for deep suboccipital and levator scapulae trigger points inaccessible to manual pressure alone
- Cervical joint mobilisation (C1–C3) — graded manual techniques to restore articular mobility and reduce facet joint irritation
- Soft tissue massage — myofascial release of the cervical extensor chain to decompress chronically overloaded tissues
- Taping (Kinesio or rigid) — postural facilitation taping to cue correct head position during work hours
Corrective Exercise & Ergonomic Retraining
- Deep cervical flexor (DCF) reactivation — chin-tuck and longus colli activation exercises to restore the deep stabiliser function lost in forward-head posture
- Scapular retraction and depression exercises — counteracts the rounded shoulder posture that loads the upper trapezius and levator scapulae
- Suboccipital self-release protocol — therapy ball technique taught for daily home use between sessions
- Monitor height and screen distance correction — specific guidance for Sungai Buloh office setups and WFH workstations
- Structured movement breaks — evidence-based micro-break protocol with frequency and duration calibrated to work schedule
Red Flags: When to See a Doctor Immediately (Not Just a Physiotherapist)
Do not self-manage your headache if any of the following are present:
- Sudden, “thunderclap” onset headache — the worst headache of your life appearing in seconds — possible subarachnoid haemorrhage
- Headache accompanied by fever, stiff neck, and sensitivity to light — possible meningitis
- New headache in a patient over 50 years old with no prior history — requires medical investigation
- Headache associated with visual disturbances, speech difficulty, or limb weakness — possible neurological emergency
- Headache worsening progressively over days or weeks without any musculoskeletal trigger
- Unexplained weight loss, night sweats, or fever alongside head or neck pain — possible systemic or neoplastic cause
📍 Local Note: This guide is written for patients in Sungai Buloh and the Klang Valley corridor. Hospitals and specialist centres nearby include Hospital Sungai Buloh (HSB), Columbia Asia Hospital Petaling Jaya, Subang Jaya Medical Centre (SJMC), and KPJ Damansara Specialist Hospital. For post-diagnosis physiotherapy, our vetted rehabilitation partners serve patients across Sungai Buloh, Kepong, Shah Alam, Petaling Jaya, Damansara, and surrounding areas.
Frequently Asked Questions About Tech Neck and Cervicogenic Headache in Malaysia
Both conditions produce head pain, but they differ in their origin and response to treatment. A true tension-type headache originates from central sensitisation and vascular mechanisms, and typically responds well to analgesics, rest, and stress management. A cervicogenic headache originates from a structural problem in the cervical spine — specifically tight muscles with active trigger points, stiff facet joints, or both. The defining clinical test is provocation: pressing on specific neck muscles in a cervicogenic headache will reliably reproduce your exact headache sensation. Analgesics provide only temporary, incomplete relief because they address the symptom, not the structural driver.
For most patients with cervicogenic headache from Tech Neck, a structured physiotherapy course of 6–10 sessions over 4–8 weeks produces significant or complete headache resolution. Many patients notice a measurable reduction in headache frequency and intensity after just 2–3 sessions of trigger point release and cervical mobilisation. The longer the condition has been present before treatment begins, the more sessions are typically required. Patients who simultaneously implement ergonomic changes at their workstation and perform their prescribed home exercise programme consistently tend to achieve the fastest and most durable results.
Dry needling for the cervical region and upper trapezius is generally well-tolerated. Most patients describe the insertion of the needle as minimal, and the therapeutic “local twitch response” — a brief involuntary muscle twitch that confirms the needle has engaged the trigger point — as a momentary, deep cramping sensation that resolves within seconds. Post-treatment muscle soreness for 12–24 hours is normal and is not a sign of injury. In the hands of a trained and registered physiotherapist, dry needling in the cervical region is a safe and clinically validated technique for treating suboccipital trigger points that are not adequately reached by manual compression alone.
Prolonged, uncorrected Tech Neck posture does not cause immediate structural damage, but over months to years it can contribute to accelerated cervical disc degeneration, facet joint arthropathy, and chronic myofascial pain syndrome. The good news is that the musculoskeletal effects of poor WFH ergonomics are largely reversible when addressed early. The risk window for preventable structural changes is within the first 1–3 years of sustained poor posture. Malaysian home office workers using dining tables, sofas, or low coffee tables as workstations are at particular risk because these setups force the head into sustained extreme flexion that office chairs with adjustable armrests partially mitigate.
The top edge of your monitor should be at or just below eye level, with your gaze angling slightly downward (approximately 15–20 degrees) to your primary work area. The monitor should be an arm’s length away (approximately 50–70 cm). For laptop users — the majority of Sungai Buloh’s WFH workforce — a laptop stand or external monitor combined with a separate keyboard is essential; using a laptop flat on a desk forces the head into chronic 40–50 degree flexion. Smartphone use should be brought up toward eye level as much as possible, especially for extended reading or messaging sessions.
Private physiotherapy in the Sungai Buloh and Klang Valley corridor typically costs RM 80 to RM 180 per session. A standard course for cervicogenic headache and Tech Neck (6–10 sessions) would typically total RM 600–RM 1,500. Sessions involving dry needling may carry a small surcharge at some clinics. Patients with private medical insurance should verify whether their policy includes an outpatient physiotherapy benefit. Our vetted partners can provide an itemised quote and advise on claim documentation during your first appointment.
Yes — several evidence-based self-care measures can provide meaningful interim relief. Apply a warm, moist heat pack to the base of your skull and upper neck for 15–20 minutes to relax the suboccipital muscles. Perform gentle chin-tuck exercises: while seated, gently retract your chin straight back (not down) to create a “double chin” and hold for 5 seconds, repeating 10 times every hour. Use a therapy ball or firm rubber ball pressed against the base of your skull while lying on the floor to perform sustained suboccipital compression. Avoid prolonged phone use with your head down, and raise your laptop screen if at all possible. These measures manage symptoms but do not treat the underlying trigger points — professional intervention remains necessary for resolution.
Both registered physiotherapists and chiropractors can treat cervicogenic headache and Tech Neck. In Malaysia, physiotherapists registered with the Malaysian Physiotherapy Association (MPA) offer a comprehensive approach combining trigger point release, dry needling, joint mobilisation, progressive therapeutic exercise, and ergonomic rehabilitation. The key is ensuring your practitioner is licensed under Malaysia’s Allied Health Professions Act (AHPA) and has specific post-graduate training in musculoskeletal or sports physiotherapy. Our vetted partners meet these credentials and specialise in occupational neck pain for Klang Valley corporate workers.
📅 Book Your Tech Neck Assessment in the Klang Valley
Whether you have daily headaches, persistent neck stiffness, or both, the right diagnosis is everything. Our vetted physiotherapy partners across Sungai Buloh and the Klang Valley provide accurate clinical assessment and condition-specific rehabilitation from the very first session.
Tap your location to open WhatsApp — no forms, no waiting.
The information in this article is intended for general educational purposes and does not constitute medical advice. Always consult a clinician registered with the Malaysian Medical Council (MMC) or a physiotherapist registered with the Malaysian Physiotherapy Association (MPA) for a diagnosis and personalised treatment plan. ServicePro.my connects Malaysians with vetted, verified healthcare and home service professionals across the Klang Valley and beyond.
─── MORE HEALTHCARE INSIGHTS
Keep Reading
Continue building your knowledge on maintaining a healthy community in Malaysia.