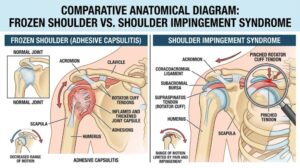
Slipped Disc Treatment in Klang Valley: Physiotherapy vs. Surgery for Sciatica
For urban professionals enduring long KL commutes and desk-bound workdays, lumbar spine injuries have quietly become one of the most common musculoskeletal complaints seen in Klang Valley private clinics. This guide gives you the clinically grounded breakdown of both treatment pathways.
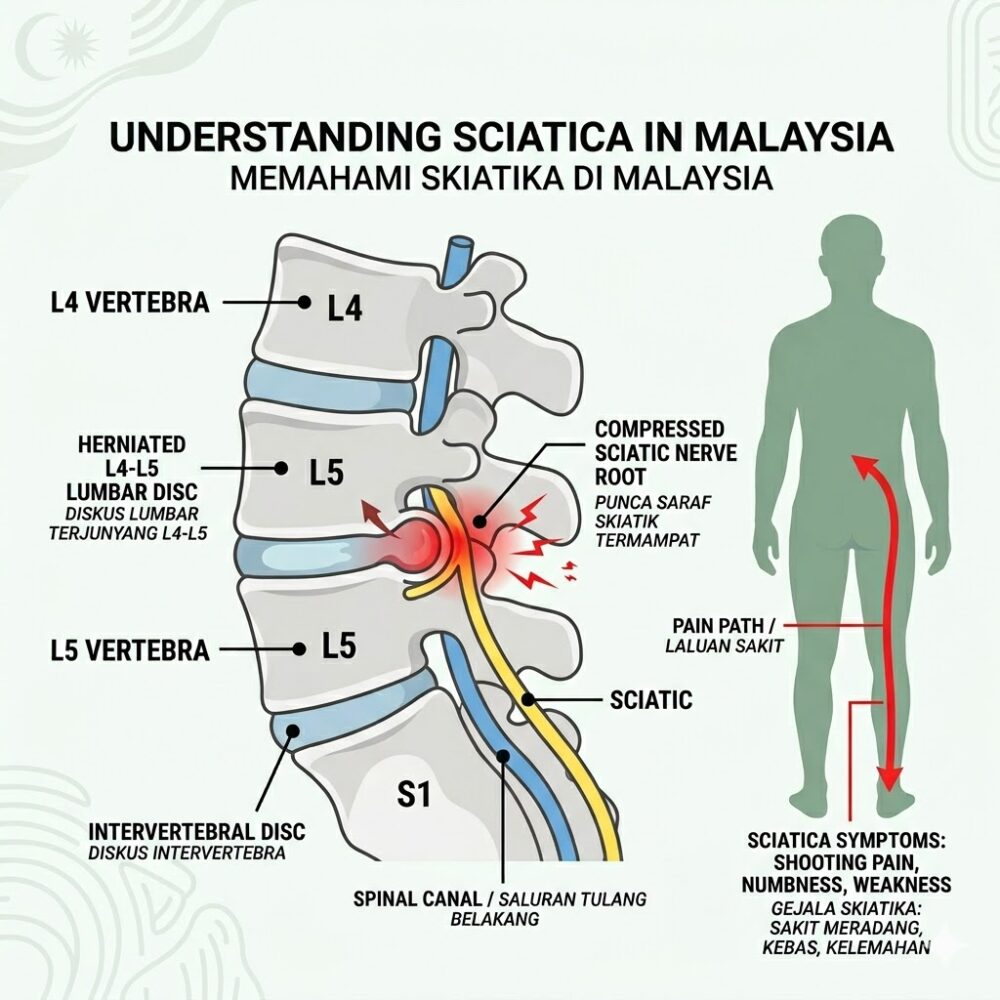
What Is a Slipped Disc, and Why Does It Cause Sciatica?
A slipped disc — clinically termed a lumbar disc herniation — occurs when the nucleus pulposus (the soft, gel-like interior of an intervertebral disc) breaches the annulus fibrosus (its tough outer casing) and protrudes into the spinal canal, directly compressing adjacent nerve roots.
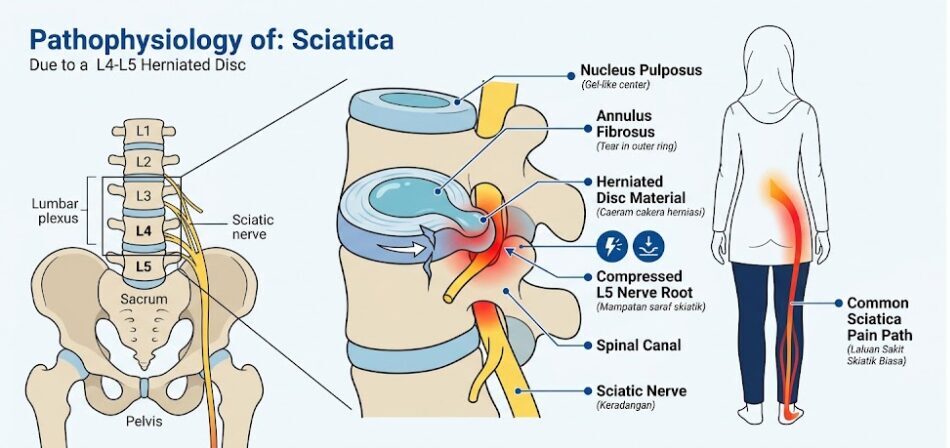
This mechanical compression, combined with the pro-inflammatory cytokines released by the exposed disc material, directly irritates the sciatic nerve — the body's longest peripheral nerve, running from the lumbar spine through the buttocks and down to the toes. The result is sciatica: a constellation of symptoms that should not be confused with ordinary lower back pain.
Classic Sciatica Symptoms Include:
Radiating Leg Pain
An electric shock or burning sensation that travels from the lower back, through the buttock, and down the posterior thigh into the calf or foot — typically affecting one side.
Dermatomal Numbness
"Pins and needles" or complete sensory loss in a specific strip of skin correlating to the compressed nerve root (commonly L4, L5, or S1).
Motor Weakness
Difficulty dorsiflexing the foot (foot drop), standing on tiptoes, or bearing weight on the affected limb.
Positional Aggravation
Sharp pain spikes during coughing, sneezing, or prolonged sitting — a daily reality for patients stuck in PJ–KL morning traffic.
Clinical Note: Not all lower back pain is a slipped disc, and not all disc herniations cause sciatica. An accurate diagnosis from a registered physiotherapist or orthopaedic specialist is essential before any treatment protocol begins.
How Is a Slipped Disc Diagnosed in Malaysia?
Slipped disc diagnosis in Malaysia combines clinical neurological testing with imaging, and an MRI scan of the lumbar spine remains the gold-standard investigation. A trained physiotherapist or orthopaedic surgeon will typically follow this diagnostic pathway:
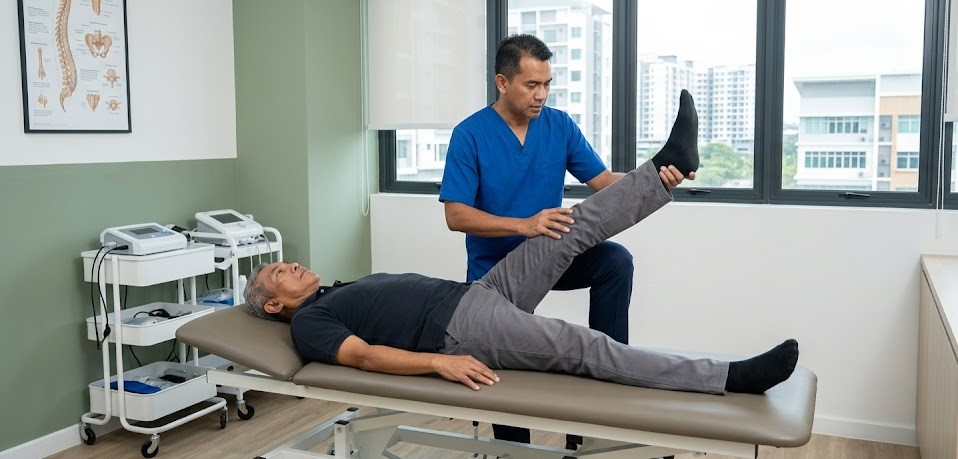
Clinical Assessment
Before any imaging is ordered, clinicians use specific provocative tests to identify nerve root involvement:
Straight Leg Raise (SLR) Test
Lifting the patient's straightened leg to 30–70° reproduces sciatic pain, indicating nerve root irritation.
Slump Test
A seated neural tension test that reproduces leg symptoms, confirming sciatic nerve involvement.
Dermatomal Mapping
Assessing sensory deficits across the leg to identify which nerve root level (L3, L4, L5, or S1) is compressed.
Myotomal Testing
Checking muscle strength at specific levels (e.g., big toe extension for L5, ankle plantarflexion for S1).
Imaging Investigations
| Investigation | Purpose | Estimated Cost in Malaysia |
|---|---|---|
| MRI Lumbar Spine | Definitive disc herniation confirmation; shows nerve compression | RM 800 – RM 1,500 |
| X-Ray (AP & Lateral) | Rules out fractures and spondylolisthesis; does not visualise soft tissue | RM 80 – RM 200 |
| CT Scan | Used when MRI is contraindicated (e.g., pacemaker patients) | RM 500 – RM 1,000 |
| Nerve Conduction Study (NCS/EMG) | Quantifies motor nerve damage; informs surgical planning | RM 400 – RM 800 |
Important: An MRI is not mandatory before beginning physiotherapy. If symptoms are consistent with a clinical diagnosis and no red flags are present, a registered physiotherapist may begin conservative treatment immediately and request imaging only if symptoms fail to progress.
Physiotherapy vs. Surgery: Which Treatment Is Right for Your Slipped Disc?
Non-invasive physiotherapy is the clinically recommended first-line treatment for the vast majority of lumbar disc herniations, with surgery reserved strictly for cases presenting with severe, progressive neurological deterioration.
Clinical guidelines from bodies including the Malaysian Orthopaedic Association (MOA) and international spinal medicine consensus groups consistently support an initial 6–12 week trial of conservative, supervised physiotherapy before surgical options are considered — unless specific "red flag" criteria are met.
If surgery is ultimately required, a dedicated post-surgical orthopedic rehabilitation programme in the Klang Valley becomes essential to restore mobility and prevent scar tissue tethering.
Side-by-Side Comparison: Physiotherapy vs. Spinal Surgery
| Criteria | Physiotherapy | Surgery (Microdiscectomy / Fusion) |
|---|---|---|
| Clinical indication | First-line for >90% of cases | Reserved for neurological red flags or physio failure |
| Invasiveness | Non-invasive | Invasive; requires general anaesthesia |
| Recovery timeline | 4–12 weeks to functional recovery | 6 weeks minimum; full recovery 3–6 months |
| Risk profile | Minimal (muscle soreness, temporary symptom flare) | Infection, nerve injury, failed back surgery syndrome (FBSS) |
| Recurrence prevention | High — addresses biomechanical root cause | Moderate — adjacent segment disease is a known risk |
| Cost (Klang Valley) | RM 1,500 – RM 3,000 for a full programme | RM 25,000 – RM 65,000 (private hospital) |
| Insurance/SOCSO coverage | Usually covered with GP/specialist referral | Usually covered under major medical plans |
| Best for | Radiating pain, numbness, lifestyle impairment | Foot drop, bladder/bowel loss, intractable pain |
Ready to Start Your Recovery? Book a Clinical Assessment Today.
Our verified PERKESO panel physiotherapy centre in Sungai Buloh serves patients across the Klang Valley. Select your nearest area to send a WhatsApp enquiry directly to Perkeso Physiotherapy Centre.
What Does Physiotherapy for a Slipped Disc Actually Involve?
A structured physiotherapy programme for lumbar disc herniation addresses nerve decompression, pain modulation, and spinal stability simultaneously — not just symptom relief.
An evidence-based programme delivered by a registered physiotherapist (registered with the Malaysian Physiotherapy Association, MPA) will typically progress through three structured phases:
Acute Pain Management
The priority in this phase is reducing neural inflammation, restoring basic mobility, and eliminating protective muscle spasm.
- Manual Therapy: Joint mobilization and soft tissue release techniques to reduce acute lumbar muscle guarding
- Modalities: Therapeutic ultrasound, interferential therapy (IFT), or TENS to modulate pain signals
- Neural Mobilisation: Gentle nerve flossing and sciatic nerve glides to reduce adhesion around the nerve root
- Postural Education: Correct sitting, standing, and sleep posture to minimise compressive load on the herniated segment
Functional Recovery
Once acute pain is controlled, rehabilitation shifts to motor retraining and spinal reconditioning.
- McKenzie Method (MDT): Directional preference exercises specifically designed to centralise pain — moving symptoms from the foot back toward the spine
- Spinal Decompression Therapy: Mechanical or manual traction applied to the lumbar spine to create negative intradiscal pressure, encouraging the herniated nucleus to retract
- Core Stabilisation Programme: Systematic activation and strengthening of the transverse abdominis, multifidus, and pelvic floor
Maintenance and Relapse Prevention
Long-term spinal health and relapse prevention through lifestyle integration.
- Ergonomic Assessment: Particularly relevant for KL and PJ-based desk workers; posture correction for prolonged sitting, laptop positioning, and car seat ergonomics
- Progressive Loading: Return to sport, gym, or demanding physical work through graded exposure
- Home Exercise Programme: A personalised, independent routine to sustain spinal health long-term
For a comprehensive, supervised rehabilitation programme, residents across Selangor and the Klang Valley can book an initial assessment at a verified slipped disc physiotherapy centre in Sungai Buloh, where certified physiotherapists conduct thorough neurological assessments and build individualized recovery roadmaps.
When Is Spinal Surgery Actually Necessary? Recognising the Red Flags
Spinal surgery for a slipped disc is medically necessary in a minority of cases — but when these clinical red flags are present, delay can result in permanent neurological damage.
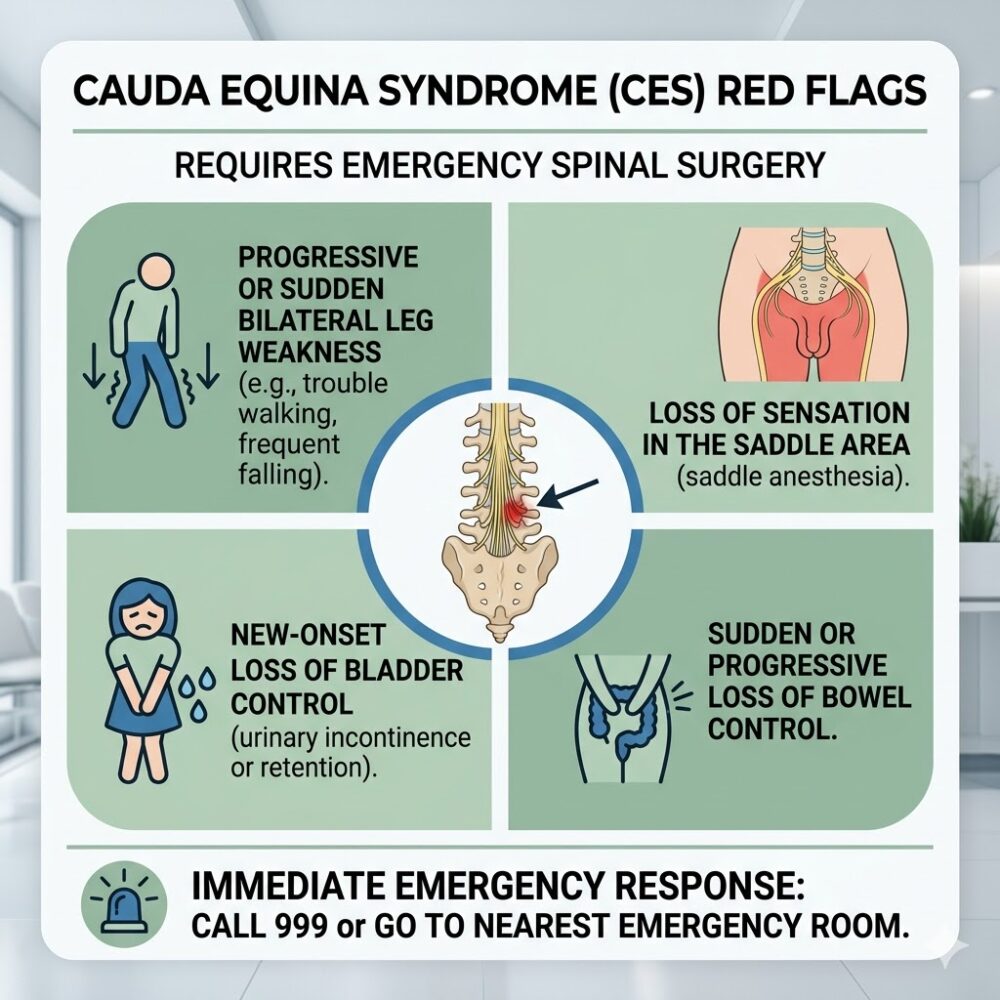
Orthopaedic surgeons and neurosurgeons in Malaysia will recommend proceeding directly to surgical intervention — bypassing the physiotherapy trial — if any of the following are present:
Absolute Surgical Emergencies — Seek A&E Immediately
- Cauda Equina Syndrome (CES): Compression of the terminal spinal nerve bundle causing bilateral leg weakness, saddle anaesthesia (numbness in the groin and inner thighs), and — critically — loss of bowel or bladder control. This is a neurosurgical emergency; irreversible damage can occur within hours if not decompressed.
- Rapidly Progressive Motor Deficit: Sudden or rapidly worsening foot drop, inability to lift the leg, or bilateral lower limb weakness indicating acute severe nerve compression.
Relative Surgical Indications — Discuss with Specialist
- Intractable, unremitting pain: Debilitating sciatica that fails to respond to a minimum of 6–8 consecutive weeks of intensive, supervised physiotherapy and appropriate pharmacological management (NSAIDs, neuropathic pain agents, epidural steroid injections).
- Confirmed large disc herniation with significant neural compromise: MRI evidence of a sequestrated or extruded fragment causing severe canal stenosis, paired with worsening clinical findings.
How Long Does Physiotherapy Take to Heal a Slipped Disc in Malaysia?
Most patients in Malaysia experience significant, measurable pain relief and functional improvement within 4 to 8 weeks of consistent, supervised physiotherapy — though full recovery timelines vary with herniation severity.
Recovery Timeline at a Glance
Pain Control
Pain controlled; nerve inflammation reduced; basic mobility restored.
Functional Return
Leg symptoms centralising; core engagement improving; return to light work.
Core Stability
Core stability restored; return to exercise; residual numbness resolving.
Long-term Independence
Independent home programme; ergonomic habits embedded; low recurrence risk.
Factors That Influence Recovery Speed
- Herniation size and type: A contained (bulging) disc typically resolves faster than a sequestrated (free fragment) herniation.
- Age and general health: Younger patients with good baseline fitness tend to recover more rapidly.
- Adherence to home exercises: Patients who consistently perform their prescribed home programme between clinic sessions recover measurably faster.
- Occupation: Sedentary desk workers or those who commute long distances — a significant portion of Klang Valley patients — face more compressive load accumulation and may require ergonomic intervention alongside physiotherapy.
How Much Does Slipped Disc Treatment Cost in Klang Valley?
Private physiotherapy for a slipped disc in the Klang Valley ranges from RM 150 to RM 300 per session, making a complete 10–15 session rehabilitation programme substantially more cost-effective than the RM 25,000 to RM 65,000 cost of private spinal surgery.
Detailed Cost Breakdown (Klang Valley, 2024)
| Treatment Pathway | Item | Estimated Cost |
|---|---|---|
| Physiotherapy | Per session (private clinic) | RM 150 – RM 300 |
| Full programme (10–15 sessions) | RM 1,500 – RM 3,000 | |
| MRI scan (if required) | RM 800 – RM 1,500 | |
| Orthopaedic specialist consultation | RM 200 – RM 400 | |
| Surgery (Private Hospital) | MRI + NCS workup | RM 1,200 – RM 2,300 |
| Neurosurgeon / orthopaedic surgeon fees | RM 5,000 – RM 15,000 | |
| Hospital admission + anaesthesia | RM 8,000 – RM 20,000 | |
| Procedure (microdiscectomy) | RM 12,000 – RM 30,000 | |
| Mandatory post-operative physiotherapy | RM 1,500 – RM 3,000 | |
| Total surgical pathway | RM 27,700 – RM 70,300 |
Insurance and SOCSO coverage: Most comprehensive private medical insurance (e.g., AIA, Prudential, Great Eastern) and PERKESO (SOCSO) cover physiotherapy when accompanied by a referral letter from a registered medical officer or specialist confirming medical necessity. Verify your plan's annual physiotherapy sub-limit before commencing treatment.
Frequently Asked Questions About Slipped Disc and Sciatica Treatment in Malaysia
Yes — the body's immune system is capable of phagocytosing (reabsorbing) herniated disc material over time, a process well-documented in clinical literature. This natural resorption is significantly accelerated by structured physiotherapy, which reduces compressive load on the disc and promotes the mechanical conditions for retraction. The majority of disc herniations resolve conservatively within 6–12 weeks with appropriate treatment.
No — aggressive traditional massage, spinal manipulation by unregistered practitioners, and unverified bone-setting are clinically contraindicated during acute disc herniation. Forceful manipulation of an inflamed, compromised disc can extrude the nucleus further into the spinal canal, worsening nerve compression and potentially precipitating cauda equina syndrome. Patients should only seek treatment from practitioners registered with the Malaysian Physiotherapy Association (MPA) or Malaysian Medical Council (MMC).
Yes, in most cases. Private medical insurance policies and PERKESO (SOCSO) both cover physiotherapy for disc herniation, provided the patient holds a formal referral letter from a registered GP or specialist confirming the medical diagnosis and necessity of physiotherapy. Check your individual plan for annual physiotherapy sub-limits (commonly RM 3,000–RM 10,000) and panel clinic restrictions.
The optimal position is lying on your side (on the non-painful side where possible) with a firm pillow placed between the knees. This maintains lumbar spine alignment and prevents the upper hip from internally rotating and pulling the spine out of neutral — which directly reduces pressure on the compressed nerve root. Avoid sleeping prone (face-down), as this hyperextends the lumbar spine and increases posterior disc pressure.
An MRI is not a prerequisite for beginning physiotherapy. A thorough clinical neurological assessment — including SLR testing, dermatomal mapping, and myotomal strength testing — is often sufficient for a registered physiotherapist to diagnose sciatica and initiate treatment. MRI is typically requested if symptoms are atypical, fail to improve after 4–6 weeks of physiotherapy, or if red flag signs emerge during treatment.
Seek immediate medical attention if you notice any of the following: pain radiating further down the leg toward the toes (centralisation is a good sign; peripheralisation is not), development of new muscle weakness such as foot drop, numbness spreading to the inner thigh and groin region (saddle anaesthesia), or — most critically — any change in your ability to control urination or bowel movements. These signs indicate progressive neurological compromise requiring urgent medical review.
Yes, significantly. Prolonged static sitting in a vehicle seat — particularly in low-slung, bucket-style car seats common to Malaysian drivers — flattens the natural lumbar lordosis and dramatically increases compressive intradiscal pressure. This is further compounded by whole-body vibration transmitted through the car chassis during prolonged highway driving. Patients with active sciatica should limit driving to under 30 minutes per session, use a lumbar support roll, and recline the seat slightly to reduce hip flexion load.
Well-delivered physiotherapy should not be acutely painful, though mild, temporary discomfort (particularly during neural mobilisation techniques) is normal and expected. Registered physiotherapists are trained to work within each patient's pain tolerance and should never force movement through severe pain. A temporary 24–48 hour increase in muscle soreness following a session is normal; a significant spike in leg symptoms after a session should be communicated to your therapist immediately.
Take the First Step — WhatsApp Physiotherapy Centre Directly.
Select your nearest location below to send a pre-filled WhatsApp enquiry. Our team will confirm appointment availability and advise on PERKESO/SOCSO claim eligibility.
📍 Local Note:
This article is produced by the ServicePro.my Healthcare Editorial Team for informational purposes only. It does not constitute medical advice. Always consult a licensed healthcare professional — including a registered physiotherapist, orthopaedic surgeon, or GP — for diagnosis and individualised treatment planning.
─── MORE HEALTHCARE INSIGHTS
Keep Reading
Continue building your knowledge on maintaining a healthy community in Malaysia.