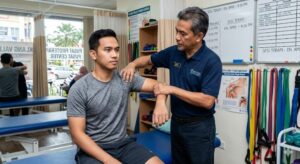
How Long Does It Take to Walk After a Stroke?
Recovery Milestones in Sungai Buloh. Regain mobility through precision neuroplasticity training and evidence-based clinical physiotherapy.
Consult a Verified Sungai Buloh Physiotherapist
How Long Does It Take to Regain Walking Ability After a Stroke?
Most stroke survivors regain the ability to walk independently within three to six months, provided they receive consistent, early-intervention physiotherapy. The exact timeline is highly individualized and depends on the severity of the stroke, the area of the brain affected, and how quickly clinical rehabilitation begins.
The brain undergoes a process called neuroplasticity — healthy regions rewire themselves to take over functions lost to damaged tissue. This rewiring is not spontaneous; it requires thousands of repetitions of specific movements. The most rapid neurological recovery occurs within the first three months post-stroke (the subacute phase), making immediate, aggressive rehabilitation the single most important clinical decision a family can make.
For patients with severe hemiparesis (one-sided body weakness), returning to unassisted ambulation may take up to a year or longer, often requiring long-term orthotic support or specialized mobility aids for elderly patients in Malaysia, such as an Ankle-Foot Orthosis (AFO).

What Are the Key Stroke Recovery Milestones for Walking?
The stroke recovery walking timeline follows a structured clinical progression — from basic bed mobility through to independent community ambulation. Physiotherapists track specific neuromuscular milestones to assess progress and adjust treatment protocols.
Core Stability & Bed Transfers
The foundation of all walking recovery is trunk control. Patients work on sitting unsupported and safely transferring to a wheelchair. Without core stability, safe standing is biologically impossible.
Standing Balance & Weight Shifting
Therapists introduce parallel bars. The patient learns equal bilateral weight-bearing and works to overcome pusher syndrome — the neurological tendency to lean toward the paralyzed side.
Gait Retraining & Assistive Devices
Stepping mechanics are retrained: hip flexion, knee control, and heel strikes. Patients transition from parallel bars to a hemi-walker or quad cane during this phase.
Community Ambulation & Endurance
The focus shifts to real-world functionality — longer distances, uneven terrain, and stairs — with the goal of discarding assistive devices where neurological recovery permits.
How Does Physiotherapy Accelerate Stroke Recovery in Malaysia?
Professional physiotherapy accelerates stroke recovery by applying high-repetition, task-specific movement therapies that directly drive neuroplasticity. Passive rest at home leads to muscle atrophy, joint contractures (permanent muscle shortening), and learned non-use of the affected limb — all of which significantly reduce long-term mobility outcomes.
Evidence-based clinical approaches used in a structured rehab setting (aligning with Ministry of Health Malaysia (MOH) clinical practice guidelines) include:
- Repetitive Task Practice (RTP): Thousands of targeted movement repetitions to force neural pathway formation.
- Constraint-Induced Movement Therapy (CIMT): Restraining the unaffected limb to compel the brain to use the weakened side.
- Neuromuscular Electrical Stimulation (NMES): Electrical impulses applied to paralyzed muscles, particularly effective for treating foot drop.
- Body-Weight-Supported Treadmill Training (BWSTT): A harness system that enables safe stepping practice before the patient can support their own full body weight.
A clinical environment provides the specialized equipment and neurological expertise that cannot be replicated at home. Consider booking a comprehensive assessment at a specialized post-stroke physiotherapy rehab centre in Sungai Buloh — where therapists specialize in post-stroke neuromuscular rehabilitation.
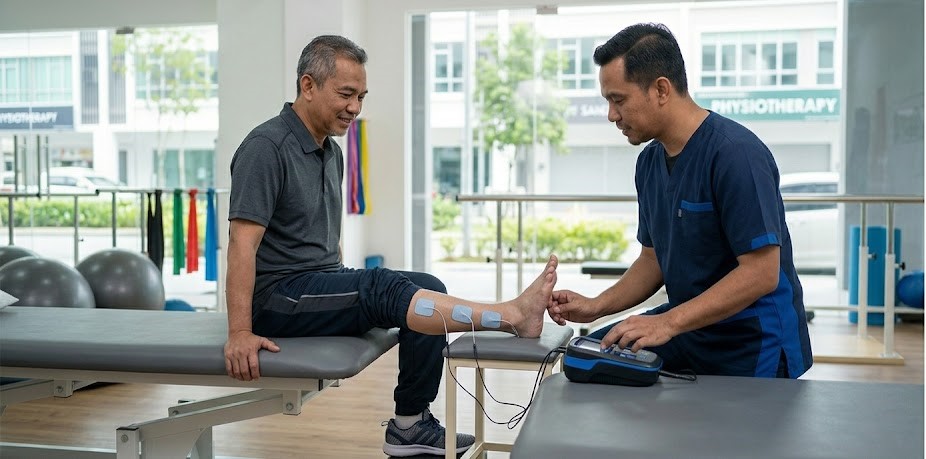
What Local Factors Affect Stroke Rehabilitation in Selangor?
Malaysia's tropical environment and residential architecture create unique rehabilitation challenges not addressed by international clinical guidelines.
- Tropical Heat and Post-Stroke Fatigue: Malaysia's high humidity severely worsens post-stroke neurological fatigue. Sessions must be conducted in air-conditioned, temperature-controlled environments to preserve patient endurance.
- Multi-Storey Terrace House Architecture: The prevalence of two- and three-storey terrace houses in Klang Valley poses an immediate barrier upon discharge. Physiotherapists must prioritize stair negotiation training early in the protocol.
- The Post-Discharge "Rehab Gap": Following acute care at certain general hospital, patients are often discharged without guaranteed continuity of therapy. Seamless transition into private outpatient care is essential to prevent neurological regression.
- Condominium Accessibility: Older high-rise condominiums in Petaling Jaya, Cheras, and Shah Alam often lack ADA-equivalent accessibility. Patients must conduct a formal home accessibility audit with their physiotherapist before discharge.

Learn About Stroke Rehabilitation Assessment Today
Our vetted physiotherapists are available across Sungai Buloh and the Klang Valley for immediate clinical assessments.
Frequently Asked Questions About Stroke Rehabilitation and Walking Recovery
Private stroke physiotherapy in the Klang Valley typically costs between RM 150 and RM 350 per session, depending on the facility's equipment and the therapist's neurological specialisation. Comprehensive monthly rehabilitation packages that bundle physiotherapy with occupational and speech therapy often provide more cost-effective structured care.
Yes, SOCSO covers rehabilitation services through their Return to Work (RTW) programme, provided the stroke is classified as an occupational disease or occurred during employment-related activity. Patients must complete a Medical Board evaluation to determine eligibility for subsidized therapy sessions and mobility aid provision.
Yes, many severe stroke survivors regain walking ability, but the process typically requires six to twelve months of intensive neurological rehabilitation. Recovery depends on the brain's neuroplastic capacity, the patient's pre-stroke cardiovascular health, and the immediate initiation of daily clinical physiotherapy. Early intervention remains the strongest single predictor of favorable mobility outcomes.
Physiotherapy should begin within 24 to 48 hours post-stroke, once the patient is medically stable as cleared by the attending neurologist. Immediate mobilization in the acute hospital setting prevents life-threatening complications including deep vein thrombosis (DVT), pressure ulcers, and rapid skeletal muscle atrophy.
Post-stroke leg stiffness is called spasticity — a condition caused by disrupted electrical signals between the damaged brain and peripheral muscles, locking them in a constant state of contraction. Management requires specialist physiotherapy interventions including targeted stretching, serial casting, and, in severe cases, Botox injections administered under physician supervision to reduce hypertonicity.
Caregivers are clinically essential for maintaining safety during home exercises, assisting with activities of daily living (ADLs), and ensuring strict adherence to the Home Exercise Programme (HEP) prescribed between clinical visits. Caregivers must be formally trained by the treating physiotherapist in safe patient-handling techniques to prevent carer back injuries during transfers and assisted standing.
Prioritise installing heavy-duty grab bars in wet bathrooms, replacing squat toilets with elevated seated commodes, and securing all loose rugs to eliminate fall hazards. In the early stages of recovery when stair navigation is unsafe, the patient's primary bedroom and living space must be fully relocated to the ground floor. A qualified physiotherapist can conduct a formal home safety assessment before discharge.
A TIA (Transient Ischaemic Attack), often called a "mini-stroke," produces temporary neurological symptoms that resolve within 24 hours without permanent tissue death. A full ischaemic or haemorrhagic stroke results in lasting brain tissue damage requiring sustained rehabilitation. TIA patients do not typically require walking rehabilitation but must undergo urgent medical investigation to prevent a subsequent, more severe stroke.
Ready to Begin? Find a Stroke Rehab Specialist Near You
Service Pro connects you with clinically vetted physiotherapists across Sungai Buloh and the Klang Valley. Tap your location to connect instantly via WhatsApp.
Tap your location to open WhatsApp — no forms, no waiting.
📍 Local Note:
This article is produced by the ServicePro.my Healthcare Editorial Team for informational purposes only. It does not constitute medical advice. Always consult a licensed healthcare professional — including a registered physiotherapist, orthopaedic surgeon, or GP — for diagnosis and individualised treatment planning.
─── MORE HEALTHCARE INSIGHTS
Keep Reading
Continue building your knowledge on maintaining a healthy community in Malaysia.