After Heart or Lung Surgery in Selangor: Why Supervised Rehab — Not Rest — Is What Your Body Needs
Recovering from CABG, valve surgery, lobectomy, or pneumonectomy? This clinical guide — written for patients and caregivers in Selangor and the Klang Valley — explains why supervised rehabilitation is the evidence-based standard of care, what the programme actually looks like, and how to start within the optimal recovery window.
Book Pre-Rehabilitation Assessment
Who this article is for: Patients recovering from coronary artery bypass grafting (CABG), valve repair or replacement, lobectomy, pneumonectomy, or lung transplant — and their caregivers — who are based in Selangor or the broader Klang Valley.
What Is Supervised Cardiac and Pulmonary Rehabilitation, and Do You Really Need It After Surgery?
Supervised cardiac and pulmonary rehabilitation is a structured, medically monitored programme of graded exercise, education, and psychosocial support designed to restore functional capacity and reduce re-hospitalisation risk after major heart or lung surgery. The short answer is: yes, you need it — and the evidence is unambiguous.
A 2023 meta-analysis published in the European Journal of Preventive Cardiology found that patients who completed a formal cardiac rehabilitation programme after CABG reduced their all-cause mortality risk by up to 26% over five years compared to those who received only standard post-discharge instructions. For post-thoracic surgery patients, pulmonary rehabilitation has been shown to recover peak VO₂ (maximal oxygen uptake) to near-baseline levels significantly faster than unassisted recovery.
Yet across Malaysia, post-surgical rehab remains chronically underutilised. Data from the National Heart Institute (Institut Jantung Negara) has consistently shown that fewer than 30% of eligible post-cardiac surgery patients in the Klang Valley complete a formal rehabilitation programme. The barrier is rarely motivation — it is access, medical oversight, and the dangerous misconception that bed rest alone is the safest path to healing.
It is not. Supervised, progressive rehabilitation is.
What Physically Happens to Your Heart and Lungs After Surgery — And Why Inactivity Makes It Worse
After open-heart surgery or thoracic (chest) surgery, your body undergoes a cascade of physiological changes that make unsupervised recovery genuinely dangerous.
Following CABG or valve surgery, the pericardium (the protective sac around the heart) is opened and manipulated. This triggers a systemic inflammatory response that can persist for weeks, elevating C-reactive protein (CRP) and creating a pro-coagulant state — meaning your blood is more prone to clotting. Simultaneously:
- Sternal instability: The breastbone (sternum) is typically wired shut after open-heart surgery, but bone healing takes 6–12 weeks. Unsupervised movement, lifting, or exertion can destabilise the sternum, a complication known as sternal dehiscence — a surgical emergency.
- Cardiac deconditioning: Even a week of bed rest causes measurable reductions in stroke volume (the amount of blood the heart ejects per beat) and cardiac output. This deconditioning accelerates rapidly in older patients.
- Pericardial effusion: Fluid can accumulate around the heart in the weeks following surgery. Moderate exertion under monitoring can reveal this; unmonitored exertion can trigger cardiac tamponade.
- Arrhythmia vulnerability: Post-surgical patients are at elevated risk for atrial fibrillation (AF), the most common complication after cardiac surgery, occurring in 25–40% of patients. Supervised rehab includes continuous ECG telemetry to detect and respond to arrhythmias in real time.
Following lobectomy (removal of a lung lobe), pneumonectomy (removal of an entire lung), or video-assisted thoracoscopic surgery (VATS), the remaining lung tissue must undergo compensatory hyperinflation — physically expanding to partially fill the space left by the resected tissue. This process, called postpneumonectomy syndrome in severe cases, benefits critically from guided breathing exercises.
- Reduced FEV₁ and FVC: Forced expiratory volume (FEV₁) and forced vital capacity (FVC) — the two primary markers of pulmonary function — drop acutely after thoracic surgery and recover on a trajectory directly influenced by early, structured breathing rehabilitation.
- Sputum retention: Post-operative patients have impaired mucociliary clearance. Retained secretions lead to pneumonia, the leading cause of post-thoracic surgery death. Supervised pulmonary rehab includes active cycle of breathing technique (ACBT) and positive expiratory pressure (PEP) therapy to clear the airways.
- Diaphragmatic dysfunction: The phrenic nerve, which controls the diaphragm, can be bruised or stretched during thoracic procedures. Diaphragmatic breathing exercises under supervision begin the process of re-establishing normal respiratory mechanics.
- Oxygen desaturation during exertion: A patient who appears stable at rest may desaturate dangerously (SpO₂ dropping below 88%) during even mild exertion. Without pulse oximetry monitoring, this goes undetected.
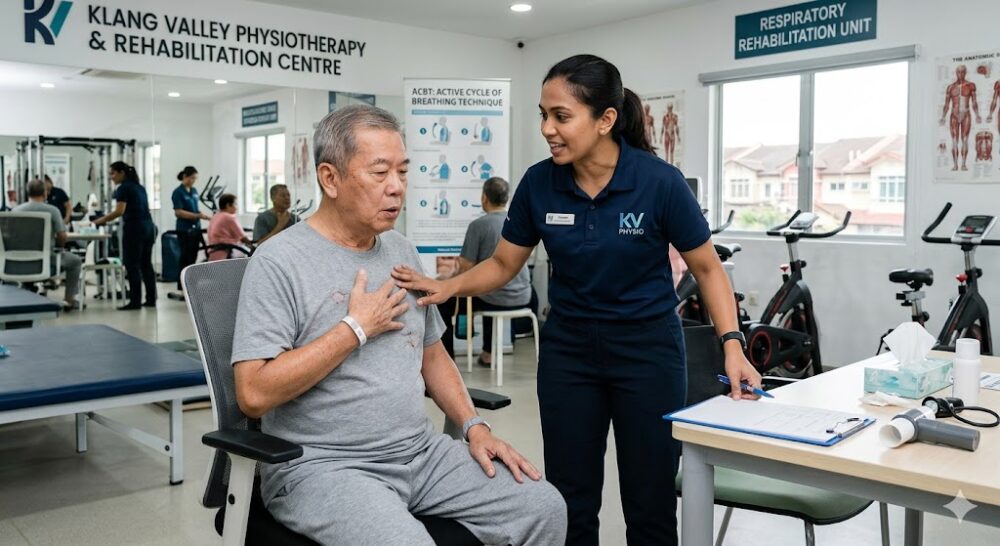 A physiotherapist demonstrating active cycle of breathing technique (ACBT) — a core intervention in supervised pulmonary rehabilitation for post-lung surgery patients in Klang Valley.
A physiotherapist demonstrating active cycle of breathing technique (ACBT) — a core intervention in supervised pulmonary rehabilitation for post-lung surgery patients in Klang Valley.Why “Just Walk More” Is Not a Rehabilitation Programme
One of the most common pieces of discharge advice given to post-surgical patients at Malaysian public hospitals is: “Walk a bit every day and come back in six weeks.” This is not a rehabilitation programme. It is discharge planning.
Here is what unstructured, self-directed recovery misses:
| What Supervised Rehab Provides | What “Walk More” at Home Provides |
|---|---|
| Real-time ECG telemetry during exertion | No cardiac monitoring |
| Continuous SpO₂ (oxygen saturation) tracking | No detection of silent desaturation |
| Graded exercise prescription (METs-based) | Arbitrary, uninformed intensity |
| Sternal precaution monitoring | No structural protection |
| Pharmacist-led medication optimisation (e.g., beta-blocker titration) | None |
| Psychosocial screening for post-cardiac surgery depression | None |
| Nutritional counselling aligned with cardiac or respiratory diet guidelines | None |
| Clinician response to arrhythmia, dyspnoea, or desaturation events | Delayed emergency response (999) |
The critical concept here is metabolic equivalent of task (MET): a physiological measure of exercise intensity. Normal walking is approximately 3.5 METs. After major cardiac surgery, some patients’ safe threshold is as low as 1.5–2.0 METs. Without a formal exercise stress test and supervised programme, the patient has no way of knowing where their safe threshold sits.
At Poliklinik Dr. Kumaran’s Integrated Care clinic, each post-surgical patient undergoes a baseline cardiopulmonary exercise test (CPET) before their programme is prescribed. This test maps their actual VO₂ peak, anaerobic threshold, and heart rate recovery — creating a personalised, physiologically anchored exercise prescription. There is no guesswork.
What the Integrated Care Rehabilitation Programme at Poliklinik Dr. Kumaran Looks Like
The supervised rehabilitation programme at Poliklinik Dr. Kumaran is structured as a 12-week, three-phase integrated care model, delivered across both in-clinic and supported home sessions. It is specifically designed for the Selangor context — including the reality that many patients in areas like Sungai Buloh, Kepong, Kota Damansara, Bukit Rahman Putra, Petaling Jaya, Shah Alam, Subang, Damansara Damai, and Rawang face significant commute challenges during recovery.
Weeks 1–4 — Medical Stabilisation and Baseline Function
Frequency: 3 sessions per week, in-clinic- Full clinical assessment by Dr. Kumaran: wound site review, spirometry (for lung patients), 6-Minute Walk Test (6MWT), resting ECG, and blood panel (including BNP for cardiac patients)
- Introduction to diaphragmatic breathing and pursed-lip breathing exercises
- Low-intensity supervised ambulation on a treadmill under ECG telemetry (target: 40–60% of heart rate reserve)
- Sternal precaution education (cardiac patients): no pushing, pulling, or lifting >1 kg; no driving
- Initiation of inspiratory muscle training (IMT) using a threshold device (lung patients)
- Medication review with Dr. Kumaran: beta-blocker dose titration, ACE inhibitor or ARB adjustment, anticoagulation management
Weeks 5–8 — Progressive Conditioning
Frequency: 3 sessions per week, mixed in-clinic and supervised home sessions- Progressive aerobic conditioning: treadmill, recumbent cycling, arm ergometry — intensity increased incrementally using Borg Rating of Perceived Exertion (RPE) scale (target: 12–14/20)
- Introduction of resistance training using resistance bands and light weights — critical for preventing sarcopenia (muscle wasting), a major complication in older Malaysian patients. (For patients also managing joint or bone procedures, see our clinical guide on post-surgical orthopedic rehabilitation in the Klang Valley.)
- Structured pulmonary hygiene sessions: ACBT, PEP device use, percussion and postural drainage (lung patients)
- Psychosocial support: screening for post-surgical depression and anxiety using validated tools (PHQ-9, GAD-7). Post-cardiac surgery depression affects 25–45% of patients and is significantly under-recognised in the Malaysian clinical setting
- Dietary counselling: heart-healthy diet planning adapted for Malaysian eating patterns (e.g., reducing santan, salt, and refined carbohydrates while maintaining cultural food preferences)
Weeks 9–12 — Independence and Maintenance
Frequency: 2 sessions per week, with full home programme- Peak exertion testing: repeat 6MWT and spirometry to quantify functional gains
- Transition to a fully self-managed, personalised Home Exercise Programme (HEP) with written and digital instructions
- Return-to-work assessment: particularly relevant for patients in physically active occupations (e.g., construction, logistics) common across Selangor industrial precincts
- Long-term risk factor education: smoking cessation (critical for lung surgery patients), lipid management, blood pressure targets, diabetes management (high prevalence in the Klang Valley population)
- Scheduling of 6-month and 12-month follow-up reviews
 A post-surgical patient completing the 6-Minute Walk Test under medical supervision — a baseline clinical assessment used at the start of every programme at Poliklinik Dr. Kumaran.
A post-surgical patient completing the 6-Minute Walk Test under medical supervision — a baseline clinical assessment used at the start of every programme at Poliklinik Dr. Kumaran.Recovering from Heart or Lung Surgery in Selangor?
Our vetted integrated care partner, Poliklinik Dr. Kumaran, offers the Klang Valley’s most comprehensive supervised post-surgical rehabilitation programme — with ECG telemetry, SpO₂ monitoring, and a full 12-week structured care pathway.
Schedule a post-surgical assessment at our Sungai Buloh rehab centreWho Qualifies for Supervised Rehab After Heart or Lung Surgery in Selangor?
Supervised cardiac or pulmonary rehabilitation is appropriate — and clinically recommended — for the following patient groups:
Cardiac Surgery Patients
- Coronary artery bypass grafting (CABG)
- Aortic valve repair or replacement
- Mitral valve repair or replacement
- Heart transplant recipients
- Patients with reduced ejection fraction (EF <40%) post-surgery
Lung Surgery Patients
- Lobectomy or segmentectomy (partial lung removal, typically for lung cancer)
- Pneumonectomy (full lung removal)
- Lung volume reduction surgery (LVRS) for emphysema
- Lung transplant recipients
- Thoracoscopic (VATS) procedures
Chronic Respiratory Conditions (Non-Surgical, Eligible for Pulmonary Rehab)
- Chronic Obstructive Pulmonary Disease (COPD), particularly Stages 2–4
- Bronchiectasis
- Occupational lung disease — including among Malaysian workers with history of silica dust exposure in construction or quarrying industries
🔗 Patients managing respiratory conditions worsened by indoor air quality should also review our guide on professional mould remediation services in Malaysia, as Aspergillus and Stachybotrys spore loads in humid Malaysian homes can trigger severe exacerbations in post-surgical respiratory patients.
When Rehab Should Be Deferred (Red Flags)
- Unstable angina or acute decompensated heart failure
- Active wound infection at the surgical site
- Uncontrolled arrhythmia (e.g., resting AF with rapid ventricular response)
- Severe aortic stenosis (unoperated)
- Resting SpO₂ below 88% without supplemental oxygen
- Acute DVT or pulmonary embolism within 3 months
Dr. Kumaran conducts a full pre-programme clearance assessment to confirm eligibility before any supervised exercise begins.
How Long Does Recovery Take? A Realistic, Phase-by-Phase Timeline
Recovery timelines in Malaysia are often poorly communicated at discharge, leading to unrealistic expectations. The following reflects evidence-based benchmarks adjusted for the tropical context — high heat and humidity in Selangor can reduce exercise tolerance by 10–15%, and this is factored into the Poliklinik’s programme pacing.
| Recovery Milestone | CABG / Valve Surgery | Lobectomy / VATS | Pneumonectomy |
|---|---|---|---|
| Discharge from hospital | 5–10 days | 3–7 days | 7–14 days |
| Begin outpatient supervised rehab | Week 2–4 | Week 2–3 | Week 3–5 |
| Return to light desk work | Week 6–8 | Week 4–6 | Week 8–10 |
| Drive again (sternal clearance) | Week 6–8 | Week 3–4 | Week 4–6 |
| Return to moderate physical activity | Week 10–12 | Week 8–10 | Week 12–16 |
| Full functional independence target | 3–6 months | 2–4 months | 4–8 months |
| Complete pulmonary function recovery | N/A | 3–6 months | Permanent partial reduction |
📌 Note for Selangor patients: Malaysia’s haze season (typically August–October, influenced by Sumatera fire activity tracked by MetMalaysia and DOE) represents a high-risk period for post-surgical respiratory patients. PM2.5 levels exceeding 100 µg/m³ (Moderate to Unhealthy on the Malaysian API scale) warrant shifting outdoor exercise sessions fully indoors. The Poliklinik Dr. Kumaran facility is equipped with HEPA H13-filtered air to ensure clean air during in-clinic sessions during haze events.
The Malaysian Healthcare Gap: Why So Few Post-Surgical Patients Complete Rehab
The rehabilitation gap in Malaysia is a systemic problem, not a patient motivation problem. Understanding it helps post-surgical patients and their families advocate for themselves.
1. Public Hospital Discharge Protocols
Malaysian public hospitals — including Hospital Kuala Lumpur (HKL), Hospital Selayang, and Hospital Sungai Buloh — typically do not have sufficient outpatient cardiac or pulmonary rehabilitation capacity to serve all eligible patients. Waiting lists for structured programmes at tertiary centres can run 8–14 weeks. By that point, the optimal early rehabilitation window has partially closed.
2. Private Hospital Rehab Gaps
Many private hospitals in the Klang Valley offer in-patient physiotherapy during the admission period but do not have structured 12-week outpatient follow-up programmes. Patients are discharged with a referral letter but no programme.
3. Cost and Insurance
Many Malaysian private medical insurance (PMI) plans cover surgical procedures but explicitly exclude outpatient rehabilitation from coverage. Patients are often unaware that outpatient physio and supervised exercise at a poliklinik setting is significantly more cost-effective than a hospital-based programme — and equally clinically rigorous when delivered by a credentialed team.
4. Cultural Tendency Toward Rest
Across Klang Valley communities, there is a deeply embedded cultural belief — reinforced by family members — that post-surgery patients should rest completely and avoid exertion. Caregivers who prevent their loved ones from participating in supervised exercise, however well-intentioned, are inadvertently increasing the risk of deconditioning, depression, and re-hospitalisation.
Frequently Asked Questions About Post-Surgery Cardiac and Pulmonary Rehabilitation in Selangor
Most patients can begin outpatient supervised rehabilitation 2–4 weeks after cardiac surgery, provided they have been cleared by their operating surgeon and have no active wound complications or unstable arrhythmia. Dr. Kumaran conducts a pre-programme clearance assessment to confirm readiness before exercise begins — no self-referral exercise is attempted before this assessment.
Coverage varies significantly by insurer and plan. Some PMI plans — including those with Great Eastern, AIA, and Prudential — cover outpatient specialist consultations that include supervised rehabilitation components when prescribed by a registered physician. Patients should request a formal referral letter from their surgeon and submit a prior authorisation request to their insurer. Poliklinik Dr. Kumaran can assist with the necessary documentation.
Cardiac rehabilitation focuses on restoring cardiovascular function after heart surgery or myocardial infarction, with emphasis on aerobic conditioning, ECG monitoring, and cardiac risk factor reduction. Pulmonary rehabilitation focuses on improving lung function, airway clearance, and respiratory muscle strength after lung surgery or in chronic respiratory conditions like COPD. The Integrated Care model at Poliklinik Dr. Kumaran delivers both under one programme for patients who require combined cardiopulmonary rehabilitation (e.g., post-coronary bypass patients with concurrent COPD).
Home exercise is a component of rehabilitation — specifically in Phases 2 and 3 — but it cannot replace the medically supervised phase. The reason is clinical safety: patients in the first 4–6 weeks post-surgery require real-time ECG and SpO₂ monitoring during exertion, which cannot be delivered at home without medical-grade remote monitoring technology. A home programme alone during this window significantly increases the risk of undetected arrhythmia, dangerous desaturation, or sternal destabilisation.
Poliklinik-based outpatient rehabilitation is substantially more affordable than hospital-based programmes. As a general benchmark, structured outpatient cardiac rehabilitation at a tertiary private hospital in KL can cost RM 300–600 per session, while the equivalent programme at a specialist poliklinik typically ranges from RM 80–200 per session depending on what is included. A full 12-week programme at the poliklinik level is typically RM 3,000–8,000 total — versus RM 15,000–30,000+ at a private hospital setting. Contact Poliklinik Dr. Kumaran directly for a programme quote.
Yes — in fact, supervised rehabilitation is especially important for diabetic post-cardiac surgery patients. Exercise improves insulin sensitivity, reduces HbA1c, and lowers the cardiovascular risk multiplier that diabetes creates. However, diabetic patients require additional monitoring during sessions: blood glucose should be checked before and after exercise, and sessions should be paused if pre-exercise glucose is below 4.0 mmol/L or above 16.0 mmol/L. The programme at Poliklinik Dr. Kumaran incorporates glucose monitoring as a standard protocol for all diabetic patients.
Reluctance to exercise after lung surgery is extremely common and is often driven by kinesiophobia — the fear that physical exertion will cause harm or reopen the surgical site. This fear is clinically recognised and addressable. Dr. Kumaran’s team uses a motivational interviewing approach and begins with extremely low-intensity activities (as gentle as supported standing and controlled breathing) to build confidence. The goal in early sessions is not fitness — it is trust in the safety of movement.
Yes, significantly. Post-lung surgery patients have reduced respiratory reserve and are acutely vulnerable to PM2.5-related bronchospasm and airway inflammation during haze events. Post-cardiac patients face increased cardiac workload when breathing polluted air, which raises the risk of angina and arrhythmia. All supervised sessions at the Poliklinik are conducted indoors with filtered air. During high-API periods, patients are advised to use N95 masks for any outdoor movement and to monitor the Malaysia DOE Air Pollutant Index (API) at apims.doe.gov.my before any outdoor activity.
📅 Start Your Supervised Rehabilitation Programme in Selangor
If you or a family member is recovering from heart or lung surgery in the Klang Valley, the window for optimal rehabilitation outcomes begins in the first 2–4 weeks post-discharge — not months later.
The Integrated Care rehabilitation programme at Poliklinik Dr. Kumaran offers:
- Pre-programme clearance assessment with Dr. Kumaran (no GP referral required)
- ECG-monitored exercise sessions for cardiac patients
- SpO₂-monitored pulmonary exercise for lung surgery and COPD patients
- 12-week structured programme with in-clinic and home phases
- Dietary, psychosocial, and medication review under one roof
- Serving patients across Sungai Buloh, Kepong, Kota Damansara, Petaling Jaya, Shah Alam, and surrounding Selangor areas
Appointments available within 3 working days. Telehealth initial consultation available for patients who are not yet mobile enough to travel to the clinic.
The information in this article is intended for general educational purposes and does not constitute medical advice. Always consult a clinician registered with the Malaysian Medical Council (MMC) or a physiotherapist registered with the Malaysian Physiotherapy Association (MPA) for a diagnosis and personalised treatment plan. ServicePro.my connects Malaysians with vetted, verified healthcare and home service professionals across the Klang Valley and beyond.
─── MORE HEALTHCARE INSIGHTS
Keep Reading
Continue building your knowledge on maintaining a healthy community in Malaysia.




