Managing Knee Osteoarthritis Without Surgery: A Senior’s Guide to Mobility in Sungai Buloh
For the majority of Malaysian seniors, a structured non-surgical rehabilitation programme — including Magnetotherapy (PEMF), targeted physiotherapy, and weight management — can meaningfully restore daily mobility and delay or permanently avoid total knee replacement (TKR).
Consult a Verified Sungai Buloh Physiotherapist
Knee osteoarthritis does not have to end in an operating theatre. For the majority of Malaysian seniors — particularly those living in Sungai Buloh, Shah Alam, and the surrounding Selangor corridor — a structured, non-surgical rehabilitation programme can meaningfully restore daily mobility, reduce chronic pain, and delay or permanently avoid the need for total knee replacement (TKR).
This guide explains the clinical evidence, the therapies available locally, and the practical steps a pensioner or their caregiver can take today.
 Senior Malaysian woman performing physiotherapy knee exercises with a therapist in a Sungai Buloh rehabilitation clinic.
Senior Malaysian woman performing physiotherapy knee exercises with a therapist in a Sungai Buloh rehabilitation clinic.What Is Knee Osteoarthritis and Why Are Malaysian Seniors at Higher Risk?
Knee osteoarthritis (OA) is a degenerative joint condition in which the protective cartilage on the ends of the knee bones gradually wears away, causing pain, stiffness, and swelling. It is the most common form of arthritis among adults over 60 in Malaysia and is classified by the Ministry of Health (MOH) Malaysia as one of the leading causes of disability in the elderly population.
Why Malaysian Seniors Face Compounding Risk Factors
Malaysian seniors carry a uniquely high burden of knee OA due to a convergence of lifestyle, cultural, and environmental factors:
- High-impact daily postures: Years of squatting for solat (prayer), using squat-style toilets, or sitting cross-legged on the floor accelerate cartilage wear at the patellofemoral joint.
- Elevated BMI rates: Malaysia’s adult obesity rate — among the highest in Southeast Asia according to the National Health and Morbidity Survey (NHMS) — places chronic excess load on the medial compartment of the knee.
- Tropical humidity: Sustained high ambient humidity and barometric pressure changes (particularly during the northeast monsoon season) are strongly associated with increased joint pain sensitivity in OA patients.
- Late-stage diagnosis: Many Malaysian pensioners normalise knee pain as “sakit tua” (old age pain), presenting to clinicians only when OA has progressed to Kellgren-Lawrence Grade 3 or 4, where conservative care is more challenging.
- High-rise condo living: Seniors in high-density condominiums in Kota Damansara, Kepong, and surrounding townships who rely on stairs due to lift downtime subject arthritic knees to high-impact repetitive loading.
Clinical Grading Reference: Kellgren-Lawrence Scale
| Grade | Description | Surgical Indication? |
|---|---|---|
| 1 | Doubtful narrowing, possible osteophytes | No |
| 2 | Definite osteophytes, possible narrowing | No |
| 3 | Moderate narrowing, multiple osteophytes | Rarely |
| 4 | Severe narrowing, large osteophytes, bone deformity | Possible |
Can Knee Osteoarthritis Be Managed Without Surgery in Malaysia?
Yes — clinical guidelines from both the Malaysian Orthopaedic Association (MOA) and international bodies (NICE, OARSI) confirm that non-surgical management is the first-line, evidence-based treatment for Grades 1 through 3 knee OA. Surgery (specifically total knee replacement) is typically considered only after a structured 6-to-12-month conservative treatment programme has not produced adequate functional improvement.
The Conservative Management Hierarchy for Malaysian Seniors
A comprehensive, non-surgical plan typically integrates four pillars:
Structured Physiotherapy
Targeted strengthening of the quadriceps, hamstrings, and hip abductors to offload the damaged joint compartment.
Electrophysical Agent Therapy
Technologies including Magnetotherapy (PEMF), Therapeutic Ultrasound, and TENS used to reduce inflammation and accelerate tissue repair at the cellular level.
Weight Management & Nutritional Guidance
A 10% reduction in body weight can decrease knee joint load by up to 40% during walking — a primary intervention target for Malaysian OA patients.
Activity Modification & Assistive Devices
Customised knee orthotics, walking aids, and ergonomic advice tailored to the patient’s home environment (including terrace house vs. condominium configurations).
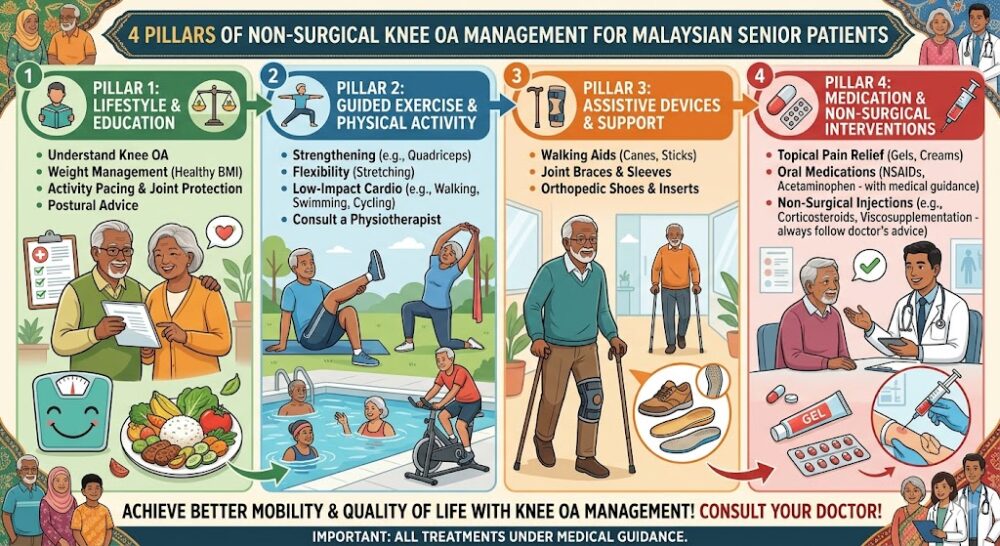 The four non-surgical pillars of knee OA management recommended for Malaysian senior patients.
The four non-surgical pillars of knee OA management recommended for Malaysian senior patients.What Is Magnetotherapy (PEMF) and How Does It Reduce Knee Joint Inflammation?
Magnetotherapy, also known as Pulsed Electromagnetic Field (PEMF) therapy, is a non-invasive electrophysical treatment that uses low-frequency electromagnetic pulses to stimulate cellular repair, reduce synovial inflammation, and inhibit pain signalling within arthritic joints.
It is one of the most clinically substantiated non-pharmacological interventions for knee OA and is increasingly adopted in geriatric rehabilitation centres across the Klang Valley, including facilities in Sungai Buloh and Subang Jaya.
How PEMF Works at the Cellular Level
The electromagnetic pulses penetrate deep into joint tissue (unlike surface-level modalities such as heat packs), acting on the following mechanisms:
Chondrocyte Stimulation
PEMF promotes the activity of chondrocytes — the cells responsible for maintaining and regenerating cartilage matrix. This is particularly significant in early-to-moderate OA where some cartilage remains.
Nitric Oxide Upregulation
The therapy increases nitric oxide production, which inhibits the pro-inflammatory cytokines (IL-1β, TNF-α) that drive cartilage degradation in OA.
Osteoblast Activation
PEMF supports bone remodelling at the subchondral bone level, addressing the bony component of OA that often causes the deep, aching pain seniors describe as “bone pain.”
Systemic Pain Gate Modulation
At the neurological level, PEMF alters the pain gate mechanism in the spinal cord, reducing the chronic pain perception that often leads to avoidance behaviour and further deconditioning.
What Does a PEMF Session Look Like for a Senior?
Important: PEMF is contraindicated for patients with cardiac pacemakers, active implanted devices, or pregnancy. Seniors with these conditions should discuss alternative modalities with their treating physiotherapist.
Evidence Snapshot: A 2022 systematic review published in Frontiers in Medicine found that PEMF therapy significantly reduced both pain scores (VAS) and stiffness in knee OA patients compared to sham treatment, with effects that persisted at 3-month follow-up — making it a durable, not just symptomatic, intervention.
 PEMF magnetotherapy device positioned over the knee of an elderly patient in a Malaysian physiotherapy clinic.
PEMF magnetotherapy device positioned over the knee of an elderly patient in a Malaysian physiotherapy clinic.What Does a Geriatric Rehabilitation Programme for Knee OA Look Like in Sungai Buloh?
A geriatric rehabilitation programme for knee osteoarthritis in Sungai Buloh is a structured, multidisciplinary plan — typically spanning 8 to 16 weeks — that combines physiotherapy, electrophysical agents (including PEMF), functional mobility training, and caregiver education to restore safe independence for the senior patient.
The distinction between a standard physiotherapy appointment and a true geriatric rehab programme is important for caregivers to understand:
Phase 1: Assessment & Baseline (Week 1–2)
- Functional mobility screening (Timed Up and Go test, 30-Second Chair Stand test)
- Pain mapping and Kellgren-Lawrence grade confirmation
- Falls risk assessment — critical, as knee OA triples the risk of falls in seniors
- Home environment assessment (stair count, toilet height, bed height)
Phase 2: Pain Reduction & Joint Preparation (Week 2–6)
- PEMF sessions (2–3x per week) to reduce baseline synovial inflammation
- Manual therapy for joint mobilisation and soft-tissue release
- Hydrotherapy referral where available (warm water reduces joint load by ~60% during exercise)
- Anti-inflammatory lifestyle counselling (dietary guidance, sleep posture)
Phase 3: Strengthening & Functional Retraining (Week 6–12)
- Progressive resistance exercises targeting VMO (Vastus Medialis Oblique) — the inner quadriceps muscle most predictive of knee stability in OA
- Balance and proprioception training (vital for fall prevention on Malaysia’s uneven pavement surfaces)
- Functional task training: safe stair negotiation, rising from low sofas, navigating wet market terrain
Phase 4: Discharge Planning & Maintenance (Week 12–16)
- Home exercise programme with clear printed instructions (in Bahasa Malaysia where required)
- Caregiver training on safe mobility assistance techniques
- Review schedule and early warning signs for OA progression
To begin a personalised, clinician-matched geriatric rehabilitation programme near Sungai Buloh, you can consult a verified geriatric physiotherapy and rehabilitation centre in Sungai Buloh through ServicePro.my’s verified partner network and be connected to a registered physiotherapist within your area.
 A caregiver assisting an elderly Malaysian man through a supervised balance exercise in a Sungai Buloh rehabilitation clinic setting.
A caregiver assisting an elderly Malaysian man through a supervised balance exercise in a Sungai Buloh rehabilitation clinic setting.Safe Exercises for Seniors with Knee OA in Malaysia’s Climate
The safest and most effective exercises for seniors with knee osteoarthritis are low-impact, closed-chain movements that strengthen the surrounding musculature without compressing the damaged joint surface — these can be performed at home or at a community park, even in Malaysia’s heat and humidity.
Perform these exercises in the morning, before Malaysia’s midday heat peaks. Hydrate well — dehydration thickens synovial fluid, increasing joint friction.
Seated Knee Extension (VMO Strengthener)
Sit upright in a firm chair (dining chair, bukan sofa yang rendah). Slowly straighten one leg until it is parallel to the floor. Hold for 5 seconds; lower slowly. 3 sets of 10 reps, each leg.
Directly strengthens the VMO without placing compressive load on the joint.
Standing Wall Slide (Mini Squat)
Stand with back flat against a wall, feet 30cm from the wall. Slide down only until thighs are at a 30° angle (not a full squat — avoid squatting deeply with OA). Hold 5 seconds; slide back up. 2 sets of 8 reps.
Builds quadriceps strength while the wall offloads spinal and knee compressive forces.
Calf Raises (Circulation & Proprioception)
Stand behind a chair, hands lightly on backrest for balance. Rise onto toes; hold 3 seconds; lower slowly. 3 sets of 15 reps.
Improves ankle proprioception, reducing falls risk, and drives venous return to reduce knee swelling.
Supine Straight Leg Raise
Lie on a firm mattress or yoga mat (not a soft tilam). Keep one knee bent; raise the straight leg to 45°; hold 5 seconds; lower slowly. 3 sets of 10 reps.
Strengthens hip flexors and quadriceps with zero knee joint load — ideal during pain flares.
Exercises to AVOID with Knee OA
- Full deep squats (bending past 90° of knee flexion)
- Stair climbing repetitions as “exercise”
- Running or jogging on concrete surfaces
- High-impact aerobics or Zumba classes (without modification)
- Cycling with the seat set too low (increases patellofemoral compression)
When Should a Senior Consider Surgery Instead of Rehabilitation?
Surgery — specifically total knee replacement (TKR) — should be considered only when a senior has completed a minimum 6-month structured conservative rehabilitation programme and continues to experience pain that severely limits daily function, or when imaging confirms Kellgren-Lawrence Grade 4 OA with significant joint space loss and bone-on-bone contact.
If surgery is ultimately required, transitioning to a dedicated post-surgical orthopedic rehabilitation programme in the Klang Valley will become the essential next step to restore joint mobility.
The decision is never purely radiological. A Kellgren-Lawrence Grade 4 X-ray finding alone is not a surgical mandate. Many Malaysian seniors with Grade 4 findings on imaging report only moderate functional limitation and manage well with ongoing conservative care.
Red Flags That Warrant Urgent Orthopaedic Referral
Caregivers should escalate care to an orthopaedic surgeon registered with the Malaysian Medical Council (MMC) if the senior experiences:
- Sudden, severe increase in knee pain not explained by activity change
- Significant joint effusion (swelling) that does not resolve within 48–72 hours
- Knee “locking” — the joint literally cannot be straightened or bent
- Vascular or neurological symptoms (numbness, tingling, pallor) in the leg or foot
- Inability to weight-bear at all, even with a walking aid
📍 Local Note: This guide is written for patients in Sungai Buloh and the Klang Valley corridor. Hospitals and specialist centres nearby include Hospital Sungai Buloh (HSB), Columbia Asia Hospital Petaling Jaya, Subang Jaya Medical Centre (SJMC), and KPJ Damansara Specialist Hospital. For post-diagnosis physiotherapy and geriatric rehabilitation, our vetted partners serve patients across Sungai Buloh, Kepong, Shah Alam, Petaling Jaya, and surrounding areas.
Not Sure If Your Knee Pain Needs Surgery?
Our vetted physiotherapy and geriatric rehabilitation partners in Sungai Buloh and the Klang Valley provide accurate clinical assessment and condition-specific non-surgical treatment — so you start the right programme from day one.
Book Knee Pain Rehab in Sungai BulohFrequently Asked Questions About Knee Osteoarthritis Management in Malaysia
Private physiotherapy sessions for knee OA in Sungai Buloh and surrounding Selangor areas typically cost between RM 80 and RM 200 per session, depending on the modalities used and the clinic’s credentials. Packages incorporating PEMF, manual therapy, and exercise supervision tend to be priced at the higher end. Seniors covered by Perkeso (SOCSO) disability schemes or government pensioner benefits under Jabatan Perkhidmatan Awam (JPA) should confirm whether their policy covers outpatient allied health services.
PEMF is contraindicated for patients with implanted cardiac pacemakers or defibrillators, and for those with active metallic implants near the treatment area. However, for seniors with non-implant cardiovascular conditions (hypertension, managed heart disease), PEMF is generally considered safe and well-tolerated. Always disclose your full medical history, including all medications, to your treating physiotherapist before beginning PEMF therapy.
Knee osteoarthritis cartilage damage cannot be fully reversed by rehabilitation alone — cartilage has very limited self-repair capacity. However, structured rehabilitation can significantly slow disease progression, reduce pain, improve functional mobility, and in many cases, postpone or eliminate the need for surgery indefinitely. The goal is functional restoration and quality of life, not radiological reversal.
Most seniors with knee OA begin to notice meaningful pain reduction after 6 to 8 PEMF sessions, with optimal results typically achieved after a full course of 12 to 15 sessions. Research indicates that the anti-inflammatory and chondroprotective effects continue to accumulate for 4 to 8 weeks after the course ends. Maintenance sessions every 4 to 6 weeks are often recommended for chronic OA management.
Yes — Hospital Sungai Buloh, a Ministry of Health (MOH) referral hospital, operates a Physiotherapy and Occupational Therapy Department that provides outpatient knee OA rehabilitation services for eligible Malaysian citizens at subsidised rates. A referral letter from a government Klinik Kesihatan or general practitioner is typically required. Wait times at public facilities can be lengthy (several weeks to months); private clinics within ServicePro.my’s partner network offer faster access to initiate treatment promptly.
Yes — hydrotherapy and aquatic exercise are among the highest-recommended modalities for senior knee OA patients globally, and are particularly suitable for Malaysia’s climate. The buoyancy of water reduces effective joint load by up to 60%, allowing strengthening exercises to be performed that would be too painful on land. Several private hospitals and sports centres in Shah Alam, Damansara, and Petaling Jaya offer supervised aquatic physiotherapy programmes. Your physiotherapist can provide a referral.
Yes — there is substantial patient-reported and emerging clinical evidence that high ambient humidity and rapid barometric pressure changes (common during Malaysia’s monsoon transitions) increase perceived joint pain in OA patients. The mechanism is thought to involve changes in the pressure within the joint capsule. This does not represent disease worsening, but pain management strategies — including PEMF, warm compress application, and adjusted exercise timing — should account for these seasonal fluctuations.
Malaysian adults over the age of 50, particularly women post-menopause and individuals with a BMI above 27.5, should discuss proactive knee OA screening with their GP or a physiotherapist. Early detection (Grade 1–2) allows intervention at a stage when cartilage preservation strategies are most effective and lifestyle modifications can have the greatest long-term impact on slowing disease progression.
📅 Book Your Geriatric Knee OA Assessment in the Klang Valley
Whether you suspect early-stage OA or have been told surgery may be needed, a structured clinical assessment is the first step. Our vetted physiotherapy and geriatric rehabilitation partners across Sungai Buloh and the Klang Valley provide accurate diagnosis and condition-specific non-surgical rehabilitation from the very first session.
The information in this article is intended for general educational purposes and does not constitute medical advice. Always consult a clinician registered with the Malaysian Medical Council (MMC) or a physiotherapist registered with the Malaysian Physiotherapy Association (MPA) for a diagnosis and personalised treatment plan. ServicePro.my connects Malaysians with vetted, verified healthcare and home service professionals across the Klang Valley and beyond.
